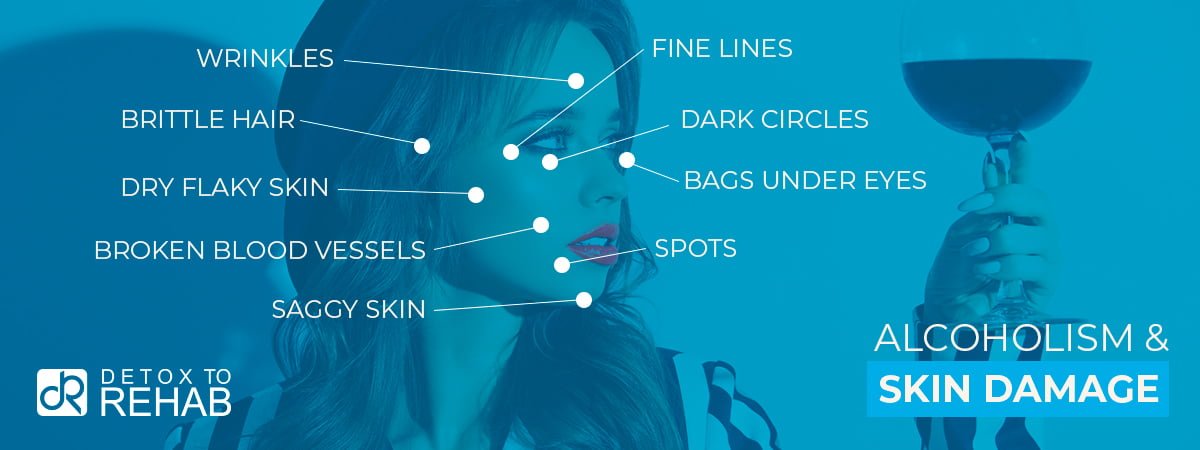
Skin Damage Issues of an Alcoholic
Alcoholism can profoundly impact skin health, manifesting in various detrimental ways. Excessive alcohol consumption leads to dehydration, promoting dry, dull, and flaky skin, accelerating the aging process with premature wrinkles and loss of elasticity. It exacerbates inflammatory skin conditions like rosacea and psoriasis, induces facial redness, and can cause spider veins due to vascular dilation. Chronic drinking disrupts nutrient absorption, depriving the skin of vital vitamins and antioxidants necessary for repair and rejuvenation. Moreover, alcohol’s impairment of the immune system heightens susceptibility to infections and hampers wound healing, further compromising skin integrity and appearance.
- Alcohol dehydrates the skin, potentially exacerbating conditions like eczema or psoriasis.
- It’s well-documented that up to 15% of individuals with alcohol dependency exhibit skin disorders
- It can cause facial redness, puffiness, and may exacerbate acne or rosacea.
- Chronic alcohol use can lead to premature aging, loss of collagen, and skin elasticity.
- Heavy drinking can accelerate the skin’s aging process by about 10 years.
Facial redness & Flushing
Alcoholism can lead to chronic facial redness and flushing, a direct result of alcohol’s vasodilatory effect, where it causes blood vessels to expand. This effect is particularly pronounced in the facial region. Over time, repeated dilation from frequent alcohol consumption can lead to a persistent flushing and even the development of visible blood vessels on the face, a condition known as telangiectasia. This not only affects one’s physical appearance, causing distress and self-consciousness, but can also be a precursor to more serious skin conditions like rosacea. The persistent redness may also be accompanied by a sensation of warmth or burning, adding to the physical discomfort.



Jaundice & Your Skin
Alcoholism can lead to jaundice, a condition characterized by yellowing of the skin and eyes. This occurs when excessive alcohol consumption causes liver damage, impeding the liver’s ability to process bilirubin, a yellow pigment formed from the breakdown of red blood cells. Alcoholic liver disease accounts for about 48% of cirrhosis-related deaths in the U.S. Accumulation of bilirubin in the bloodstream and tissues leads to jaundice. This is a serious indication of liver dysfunction, often signifying advanced alcoholic liver disease or cirrhosis. Jaundice associated with alcoholism is not just a cosmetic concern; it reflects significant health issues, requiring urgent medical attention to address potentially severe liver problems and prevent further life-threatening complications.



Nail changes associated Alcoholism
In individuals with chronic alcoholism, distinct nail changes can occur, notably koilonychia and Terry’s nails. Koilonychia, or spoon-shaped nails, is characterized by concave, scooped-out nail surfaces. It often indicates iron-deficiency anemia or liver disease, both common in alcoholics due to poor nutrition and liver dysfunction. Terry’s nails, where the nails take on a whitened appearance while retaining a narrow band of pink or brown at the tip, is observed in about 80% of patients with cirrhosis, a condition often resulting from chronic alcohol abuse. These nail changes are considered clinical markers and can be indicative of underlying health issues related to excessive alcohol consumption. These nail changes are not just cosmetic issues; they signify underlying health problems requiring medical evaluation and intervention.



Porphyria cutanea tarda
Porphyria Cutanea Tarda (PCT) is that it is considered the most common type of porphyria, accounting for about 80% of all porphyria cases. PCT is characterized by blistering, photosensitivity, and skin fragility, primarily affecting areas exposed to sunlight. A significant statistic is that among patients with PCT, up to 50% have a history of alcoholism. Alcohol is a recognized risk factor for PCT because it can exacerbate liver dysfunction and increase iron accumulation in the liver, both of which are key contributors to the development and severity of PCT symptoms. The liver damage induced by excessive alcohol use can significantly impair heme synthesis, thereby aggravating the porphyrin buildup that leads to the skin manifestations characteristic of PCT.



Skin cancer & Alcohol Abuse
Skin cancer and alcohol abuse is that alcohol consumption is associated with an increased risk of developing melanoma and other types of skin cancer. Research indicates that individuals who consume excessive amounts of alcohol are approximately 20% more likely to develop melanoma, the most serious type of skin cancer, compared to non-drinkers. This increased risk is thought to be due to ethanol in alcohol metabolizing into acetaldehyde, a compound that can damage DNA and prevent its repair, thereby increasing the likelihood of skin cell mutations that can lead to cancer.



Rosacea
Rosacea is a chronic skin condition characterized by facial redness, visible blood vessels, and sometimes acne-like bumps, primarily affecting the central face. While the exact cause of rosacea is unknown, it’s known to be exacerbated by various triggers, including alcohol consumption. Alcohol, particularly red wine, can induce rosacea flare-ups due to its vasodilatory effects, causing blood vessels in the face to widen and leading to increased redness and flushing. Research published in the Journal of the American Academy of Dermatology indicated that women who drank alcohol had a significantly higher risk of developing rosacea compared to non-drinkers. The study particularly highlighted that white wine and liquor were more strongly associated with a higher risk of rosacea.



Psoriasis
Psoriasis is an autoimmune skin condition characterized by red, scaly patches that can be itchy and painful. It results from an accelerated skin cell production process, leading to the buildup of skin cells on the surface. Alcohol abuse is linked to a higher risk of developing psoriasis—a condition that affects about 3% of the global population, but among those with alcohol use disorder, the prevalence can be as high as 16%. Individuals with psoriasis are often found to have higher rates of alcohol consumption compared to the general population. Studies have suggested that people with psoriasis are nearly twice as likely to be heavy drinkers. Furthermore, alcohol can interfere with the effectiveness of psoriasis treatments and may increase the risk of side effects from certain medications. Reducing or abstaining from alcohol is often advised to manage psoriasis effectively.



Seborrhoeic dermatitis
Seborrhoeic dermatitis is a common skin condition that causes red, scaly, and itchy patches, often on the scalp, face, and other oily areas of the body. While its exact cause is not fully understood, it’s believed to be linked to an inflammatory response to Malassezia yeasts that naturally inhabit the skin. Alcohol abuse can exacerbate seborrhoeic dermatitis. Alcohol consumption, particularly in excess, can trigger inflammatory responses and weaken the immune system, creating a more conducive environment for these yeasts to thrive. Additionally, alcohol’s dehydrating effects can disrupt the skin’s barrier function, further aggravating symptoms of seborrhoeic dermatitis. Reducing alcohol intake can help manage and reduce flare-ups of this condition.



Nummular dermatitis
Nummular dermatitis, also known as discoid eczema, is a chronic skin condition characterized by distinctive coin-shaped, itchy, and inflamed lesions. It typically occurs on the arms, hands, legs, and torso. While the exact cause of nummular dermatitis is unclear, factors such as dry skin, environmental irritants, and poor blood flow are known contributors. Alcoholism can exacerbate this condition. Alcohol consumption, particularly chronic and excessive intake, can lead to dehydration and poor nutrition, worsening dry skin and thus potentially triggering nummular dermatitis flare-ups. Furthermore, alcoholism can impair circulation and immune system function, both of which can negatively impact skin health and exacerbate dermatitis symptoms.



Spider Angiomas
Small, spider-like blood vessels visible under the skin, often found on the face and chest.
Eczema
Alcohol might worsen the symptoms of eczema, causing intense itchiness and dry, inflamed skin.
Palmar Erythema
Reddening of the palms, which can be a sign of liver damage associated with chronic alcohol use.
Seborrheic Dermatitis
Alcohol can worsen this condition, leading to flaky, white to yellowish scales to form on oily areas such as the scalp or inside the ear.
Alcoholic Hepatitis
Not a skin condition per se, but can lead to jaundice, spider angiomas, and other skin manifestations related to liver dysfunction.
Dangers of Alcoholism
Alcoholism, a chronic condition characterized by an inability to control or abstain from alcohol, has far-reaching consequences beyond skin issues. Physically, it can lead to severe liver damage, heart disease, brain damage, and increased risk of cancers. Mentally, it is associated with an increased incidence of depression, anxiety, and other psychiatric disorders. Chronic alcohol abuse impairs cognitive functions and decision-making abilities. Socially, alcoholism can strain relationships, leading to family conflicts, and workplace issues. It also heightens the risk of accidents and legal problems, including DUIs. The societal impact is profound, encompassing elevated healthcare costs and decreased workplace productivity, emphasizing the need for effective intervention and support systems.
Symptoms of Skin Damage from Alcoholism
Symptoms of skin damage due to alcohol abuse include persistent redness or flushing in the face, yellowing of the skin and eyes (jaundice), increased bruising or bleeding under the skin, dry or itchy patches, and in severe cases, swelling or changes in skin texture. Alcohol-induced skin conditions like psoriasis, eczema, or rosacea may worsen. Unusual nail changes, such as white nails or spoon-shaped indentations, can also indicate underlying issues. If you notice these symptoms or any sudden or severe changes in your skin’s appearance, it’s crucial to seek medical help. Early intervention can prevent further damage and address potential underlying health issues related to alcohol abuse.
FAQ’s
Q: How does alcoholism affect skin health?
A: Alcoholism can severely impact skin health by causing dehydration, which leads to dryness and premature aging. It can exacerbate inflammatory skin conditions like psoriasis and eczema, cause spider angiomas, and induce jaundice due to liver damage. Alcohol’s vasodilatory effect can also lead to facial redness and aggravate conditions like rosacea.
Q: Can alcohol consumption cause skin conditions to worsen?
A: Yes, alcohol consumption can worsen existing skin conditions. It can trigger flare-ups of psoriasis, eczema, and rosacea, and impair the skin’s natural healing processes. The immunosuppressive effect of alcohol can increase susceptibility to infections and impede recovery from skin injuries or surgeries.
Q: What is the link between alcoholism and jaundice?
A: Jaundice, characterized by yellowing of the skin and eyes, is often linked to alcoholism because excessive alcohol intake can lead to liver damage. The liver damage impedes the organ’s ability to process bilirubin, a yellow pigment produced from the breakdown of red blood cells, leading to jaundice.
Q: Are there specific skin conditions directly caused by alcoholism?
A: While alcoholism doesn’t directly cause specific skin conditions, it can lead to spider angiomas and palmar erythema. It significantly contributes to the development of conditions like jaundice from liver damage and can exacerbate many skin disorders, including psoriasis, rosacea, and eczema.
Q: How can recovery from alcoholism improve skin health?
A: Recovery from alcoholism can significantly improve skin health. Reducing alcohol intake can restore hydration, enhance the effectiveness of the immune system, improve liver function, and subsequently reduce jaundice and other alcohol-related skin issues. Over time, abstaining from alcohol can lead to clearer, more hydrated, and healthier skin, and also improve the management of existing skin conditions.
Reference Links
- American Academy of Dermatology Association: Alcoholism and Skin Problems
- National Institute on Alcohol Abuse and Alcoholism: Alcohol’s Effects on the Body
- The British Journal of Dermatology: Alcohol and Skin Disorders
- Mayo Clinic: Alcohol Use Disorder
- Healthline: How Does Alcohol Affect Your Skin?